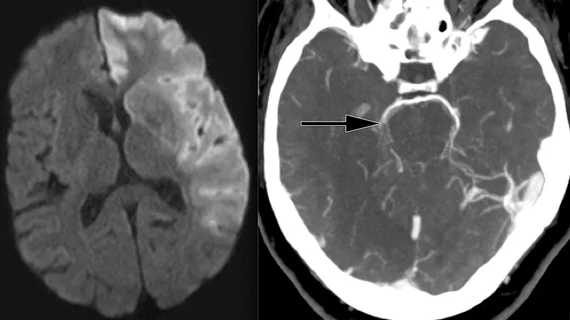
CT imaging alone found noninferior to CT/MR combo for acute ischemic stroke patients
The majority of patients who present to emergency departments under the suspicion of acute ischemic stroke are initially imaged with a combination of CT and MRI exams, but new research calls the practice into question.
On July 21, a paper published in JAMA Network Open compared the outcomes of patients with ischemic stroke who were initially evaluated with CT alone versus those who underwent both CT and MRI exams. The results of the work completed by William J. Powers, MD, of the Duke Department of Neurology at Duke University Medical Center, and colleagues indicate that CT alone is noninferior to the two-modality combo—a finding that could lead to a reduction in unnecessary imaging and waste within U.S. healthcare if validated, the experts suggested.
“Unnecessary medical imaging is a major cause of preventable waste in the US health care system,” the authors wrote. “More than 90% of patients with AIS receive MRI in addition to CT with few data to determine whether there is an associated benefit with patient outcomes.”
For their analysis of 246 patients who were hospitalized with acute ischemic stroke (AIS), the researchers determined outcomes by evaluating rates of death and/or dependence after hospital discharge and stroke or death in survivors one year after discharge.
Death or dependence at discharge occurred in 48% of patients who underwent both CT and MRI, and in 42.3% of those who completed CT exams alone. Likewise, outcomes measured at the one-year post-discharge mark revealed similar figures—death or stroke was recorded in 12.5% of patients who underwent CT alone compared to 19.5% of CT/MRI patients.
Clinical Relevance
For both outcome measures, the difference between CT alone versus a CT/MRI combo were minimal enough to meet noninferiority criteria. The experts maintained that although their results suggest that an initial imaging strategy of CT only could suffice, further research to establish the benefit of adding MRI studies to imaging protocols for patients hospitalized with AIS.
“The value of MRI added to CT in patients such as these should not be presumed,” Powers and co-authors wrote. “Further research is warranted to help determine which patients hospitalized with AIS may benefit from MRI.”
The study is available for free here.